
|
Getting your Trinity Audio player ready...
|
- Ageing arteries become less elastic, less able to regulate pressure, and are narrowed by the development of fatty deposits (atherosclerosis)
- Vascular ageing occurs due to changes within the vessel wall, including cross linking of extracellular matrix components, cellular senescence and changes in gene expression.
- Lifestyle and pharmaceutical/nutraceutical interventions aimed at lowering blood pressure are effective at slowing some aspects of this ageing process. We are also exploring ways to directly target the underlying causes of vascular ageing, such as using drugs that target senescent cells.

Age-related decline in artery function is a major contributor to cardiovascular disease which, in turn, is one of the main causes of age-related mortality.
What Changes In Ageing Arteries?
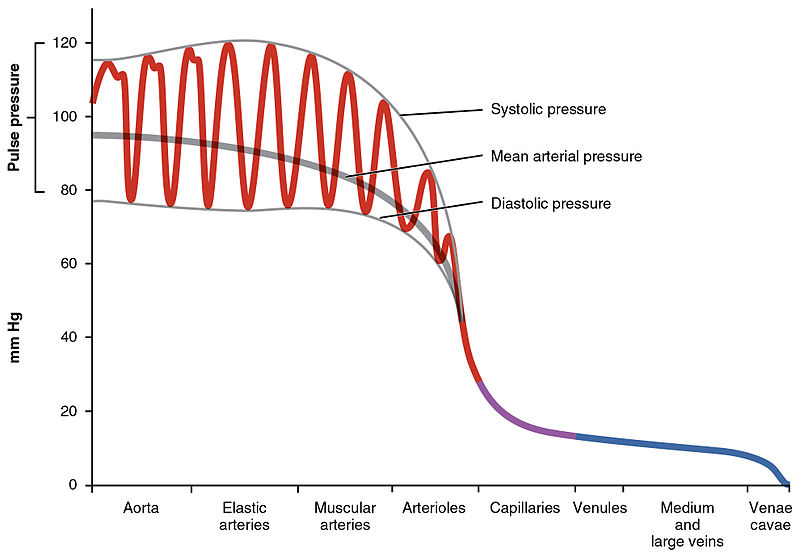
Perhaps the most important age-related change occurring in major blood vessels is a loss of elasticity. To even out the spike in pressure that occurs each time the heart contracts, arteries must be able to stretch so as to accommodate a greater volume of blood. The loss of this ability results in a rise in blood pressure that puts increasing strain on the heart, eventually leading to heart failure. Stiffening may also disrupt the way blood vessels detect and respond to pressure, which further exacerbates hypertension.
This rise in blood pressure alone is bad enough, but is made worse by the development of atherosclerosis, a process in which fatty deposits build up in the arterial walls. This not only narrows the vessels in which it occurs, but also makes the vessel wall more fragile, which can lead to various fatal events. Damage to the fatty plaque can cause a clot to form at the site of narrowing, or fat deposits can break off and block smaller vessels downstream.

What Causes These Changes?
Several factors appear to contribute to stiffening at the molecular level. The primary culprit is probably changes in the extracellular matrix (ECM), the scaffold that holds cells together. The collagen fibres that form the main component of the ECM become increasingly cross-linked with age, resulting in a loss of elasticity. Changes in gene expression with age can disrupt the regulation of ECM proteins. There is also evidence that senescent cells can contribute to vascular calcification and stiffening. Senescence is a state in which cells are no longer able divide, and if not removed by the immune system, can switch to a secretory state in which they can disrupt tissue function.
Atherosclerosis is a multi-step process that is driven by multiple age-related changes. When the wall of an artery becomes damaged (which is increasingly likely with greater blood pressure and stiffening), immune cells called macrophages are recruited to the site of damage. Once there, macrophages attempt to remove oxidised lipids that are increasingly present in the blood with age, but are unable to do so. This begins a vicious cycle of inflammation, in which more and more macrophages are recruited to clear the oxidised lipids, but ultimately make matters worse by releasing agents that oxidise more lipids. This process is exacerbated by the ageing of the immune system, which is characterised by increasing levels of inflammation.

Lifestyle factors contribute significantly to the development of atherosclerosis. For example, smoking damages blood vessels and thus accelerates the process, while high fat diets increase the rate of oxidised lipid accumulation.
How Can We Prevent Blood Vessel Ageing?
Currently, the most effective way to slow the processes described above is to avoid hypertension. Exercise and maintaining a healthy weight both lower the risk of hypertension, increase arterial compliance and protect against atherosclerosis.
Antihypertensive drugs such as diuretics, calcium channel blockers and nitrates can also reduce arterial stiffness, while statins can reduce stiffness as well as lowering inflammation in atherosclerotic plaques. There are also many supplements that may be beneficial for reducing blood pressure, reducing lipid oxidation and increasing high density lipoprotein (HDL) particles, which can remove lipids from fatty plaques.

But what about tackling the fundamental processes underlying blood vessel ageing? Several possibilities are being explored, one of which is to target senescent cells within the artery walls. As mentioned before, senescent cells seem to contribute to calcification and stiffening, but senolytic drugs designed to remove senescent cells have been shown to reduce calcification in animal models.
Other approaches involve targeting changes in gene expression that disrupt the extracellular matrix, or modulating the immune system to stop immune cells from recognising oxidised lipids.
Recommended Products
-

Weight Loss Boost
$29.99 — or subscribe and save up to 10% View Product -

Turmeric w/ Bioperine
$19.99 — or subscribe and save up to 10% View Product -

Omega 3 Fish Oil - 2500mg Lemon Flavor
$19.99 — or subscribe and save up to 10% View Product -

CoQ10 100mg
$19.99 — or subscribe and save up to 10% View Product -

Apple Cider Vinegar With Cayenne Pepper
$24.99 — or subscribe and save up to 10% View Product
References
Ageing and vascular ageing: doi: 10.1136/pgmj.2005.036053
Intrinsic stiffness of extracellular matrix increases with age in skeletal muscles of mice: https://doi.org/10.1152/japplphysiol.00256.2014
Arterial Stiffening Provides Sufficient Explanation for Primary Hypertension: https://doi.org/10.1371/journal.pcbi.1003634
Microvesicles from the plasma of elderly subjects and from senescent endothelial cells promote vascular calcification: https://doi.org/10.18632/aging.101191
Keeping the Extracellular Matrix Well Structured to Keep Healthy Vessels: https://doi.org/10.1161/ATVBAHA.118.311733
Chronic senolytic treatment alleviates established vasomotor dysfunction in aged or atherosclerotic mice: https://doi.org/10.1111/acel.12458
Copyright © Gowing Life Limited, 2024 • All rights reserved • Registered in England & Wales No. 11774353 • Registered office: Ivy Business Centre, Crown Street, Manchester, M35 9BG.


You must be logged in to post a comment.